What is Mini IVF?
As the pioneering clinic of minimal stimulation in vitro treatment, New Hope has been offering a holistic and gentle approach to Conventional IVF for over a decade.
Mini IVF uses a minimal amount of oral medication and injections to stimulate the ovaries so they produce the maximum number of “quality” eggs in a single cycle.
Our Mini IVF protocol has proven to be as successful as standard IVF treatment with over 15,000 babies born since 2004!

Mini IVF Protocol

6-8 quality eggs per cycle

Less Medication

Less Invasive
PIONEERS OF MINI IVF
In 2004 New Hope Fertility ran the very first U.S. clinical study of Mini IVF! Since then we have spent over 17 years trying to perfect the Mini IVF protocol. After years of research and constant improvement, we have managed to provide a Mini IVF that is both gentle, accessible, and highly customizable to our patients.

IS MINI IVF RIGHT FOR ME?
- Low AMH
- High FSH
- PCOS
- Poor IVF Responder
- Minimize Hormonal Medications
- Multiple Failed Conventional IVF Cycles
- Blocked or Damaged Fallopian Tubes
- LGBTQ Individuals and Couples
CONVENTIONAL IVF
NYC
$12,000
Per Cycle
22-30 Injections
Less Quality Eggs
More Invasive
MINI IVF
Starting at
$8,000
Oral pills and 1-2 Injections
6-8 Quality Eggs
Less Invasive
CONVENTIONAL
IVF NATIONAL
$20,000
Per Cycle
22-30 Injections
Less Quality Eggs
More Invasive
Mini IVF Process
A typical Mini IVF cycle takes about two weeks. The Mini IVF process consists of 4 main steps: ovulation stimulation, egg retrieval, fertilization, and finally, embryo transfer.

Step 1
Ovarian Stimulation & Monitoring
You will come in for an initial consultation and bloodwork and then your physician will build a personal treatment plan. The treatment plan will be executed and monitored over the course of two weeks.

Step 2
Egg Retrieval/Sperm Collection
The egg retrieval process is usually done with local anesthesia and takes around 10-45 minutes. The sperm collection is done on the day of the egg retrieval.
Step 3
Fertilization & Embryo Development
Fertilization of the eggs is done in a controlled laboratory setting through conventional fertilization or ICSI (Intracytoplasmic Sperm Injection).
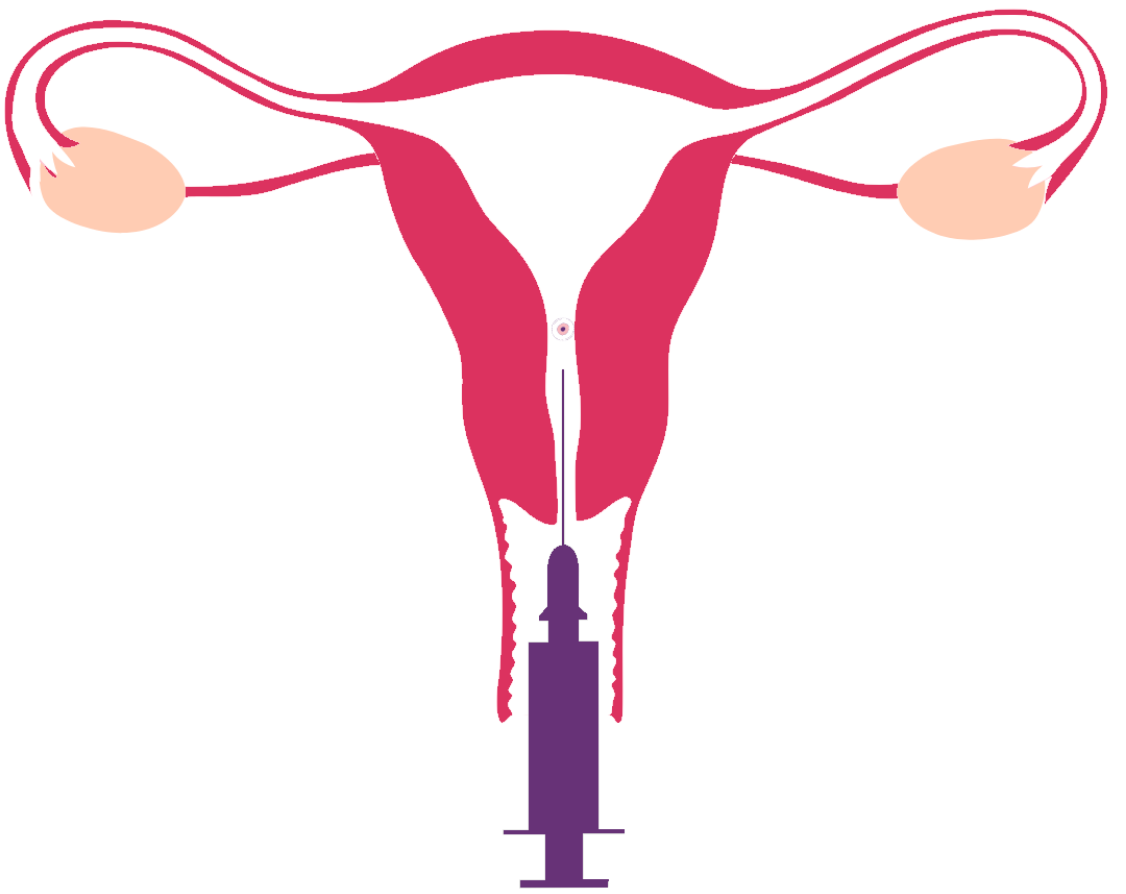
Step 4
Embryo Transfer
An embryo transfer takes about 15-20 minutes. After the embryo transfer, the patient will come into the office one week later to take a pregnancy test.
Pricing
Select respective treatment: Ovarian PRP / Uterine PRP in the price simulator.

